Piles or Haemorrhoids
Overview
Piles or Haemorrhoids are one of the most common ailments known. They are a common condition that affects 50% of the people above 50 years of age and equally in males and females. It is uncommon below the age of 20 years. Millions of Indians currently suffer from Haemorrhoids. The average person suffers in silence for a long period before seeking medical care.
Piles cause discomfort, pain, and bleeding. They can develop due to increased pressure in the lower rectum, often resulting from chronic constipation (Chronic constipation is a condition where passing stool are infrequent, difficult, or incomplete, and lasts for several months), prolonged sitting, or straining during bowel movements. Other contributing factors include obesity, pregnancy, and a low-fiber diet.
This comprehensive guide will help you explores the symptoms, causes, treatments, and preventive measures for piles and address your concerns regarding this condition effectively.
Managing piles (Haemorrhoids) can be challenging both physically and mentally. Our team of experienced and reputed A doctors and paramedical staff works dedicatedly to help you tide over your journey of piles treatment based on latest technology and evidence-based medicine. The varying nature of the disease mandates an individual need based personalised treatment plan to suit any individual and we help you prepare and execute the same for you. With over 27 years’ experience we have earned the reputation as one of the most honest and affordable treatment providers in Mumbai and around. Our thirst to upgrade our knowledge and be abreast with the latest treatment in the field has given us both national and international fame and so also patients.
What are Piles or Haemorrhoids?
The word “haemorrhoid” is derived from 2 Greek words: haema meaning blood and rhoos meaning flowing. It was probably Hippocrates (460 BC) who first used the name “haemorrhoid” to the flow of blood from the veins of the anus. It is also called “Piles”, derived from the Latin “pila” meaning a ball, and refers to the swelling that may be caused due to prolapse of the tissue. Hence, this disease is either referred to as Piles when the patient complains of swelling and Haemorrhoids when the presenting symptom is bleeding.
This condition has also been described as the “varicose veins” of the anus and rectum, but actually that’s not the case. Deterioration of the fibromuscular tissue known as the Treitz’s muscle, which supports the anal cushions, leads to sliding, engorgement, and prolapse of these cushions and consequent bleeding. These symptomatic anal cushions are referred to as Haemorrhoids.
The anal canal has 3 main cushions: left lateral, right anterior, and right posterior that correspond to the branches of the superior rectal vessels (Fig 1).
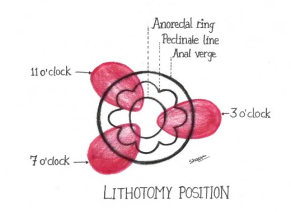
Fig 1 – Anatomy – Diagrammatic representation of anal cushions
The vascular cushions engorge following raised intrarectal pressure bringing about complete closure of the anus and maintaining continence. They also provide a protective lining for the underlying sphincters. These cushions return the anal canal lining to its original position after the temporary downward displacement that occurs during defecation.
Anal cushions are held in their normal position by the Tretiz’s muscle, as seen in the Fig 2.
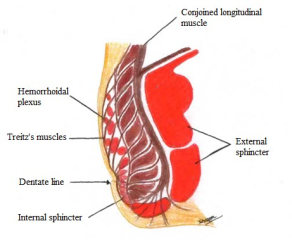
Deterioration of these tissues causes prolapse or sliding down of the cushions, resulting in venous distension, erosion, bleeding, and thrombosis. Haemorrhoids are the pathological term to describe this abnormal downward displacement of the anal cushions and subsequent venous dilatation. Piles, thus, is not “varicose veins” of the anus and rectum as some describes it.
There is a rich supply of blood in the haemorrhoidal plexus. This is one of the reasons of substantial blood loss in the patient with bleeding haemorrhoids, especially in those who are on anticoagulants.
Types of Piles or Haemorrhoids
There are mainly two types of Piles: external and internal, which refer to their location.
a) External Piles – External haemorrhoids are a perianal swelling that develops as a result of thrombosis from the inferior haemorrhoidal plexus. This normally occurs because of sudden trauma after passing hard stools or straining. They are present at the anal margins and are covered by skin. They are usually painful and seen as a small tender lump outside the anal
canal. View Fig 3 A and Fig 3 B.
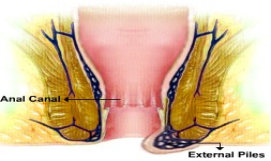
Figure 3 (A) – Diagrammatic representation of external haemorrhoids
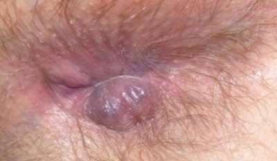
Figure 3 (B) – Formation of perianal hematoma from external hemorrhoidal plexuses
These Piles can become problematic if a blood clot — known as thrombosis — forms within them. In such cases, the affected external haemorrhoid transforms into a painful, firm lump that can cause significant discomfort. If this thrombosed pile ruptures, it may lead to bleeding, which can be alarming. Proper understanding and management of these symptoms are crucial for maintaining comfort and preventing complications.
b) Internal piles – These gets form within the anal canal, beneath the delicate lining of the rectum. They are often characterised by painless bleeding, which may manifest as bright red blood on the toilet paper or in the toilet bowl after a bowel movement. In addition to this, individuals may experience a sensation of fullness or the feeling that something is protruding (moving outside or prolapse) from the anus. However, when an internal pile becomes severely prolapsed, it extends beyond the anal opening and can no longer be reinserted manually. This condition can lead to significant discomfort and intense pain, particularly if the prolapsed tissue becomes trapped and undergoes straining or irritation. Prompt medical attention is often necessary for such cases to prevent further complications. See Fig 3 C.
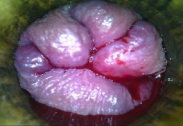
Figure 3 (C) – Active bleeding as seen in second-degree internal haemorrhoids
Internal Haemorrhoids can prolapse to varying degrees, based on which they are further classified into grades of haemorrhoids.
Grades of Piles
There are four stages of piles, formally called “grades”. These grades are:
Grade 1 – Also called as First Degree Piles. The dilated veins or the piles remain entirely within the anal canal (or the rectum) and do not bulge out of the anal opening and thus remains hidden. They might cause minor discomfort, itching, or bleeding during bowel movements.
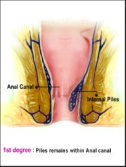
Fig 4: 1st Degree Piles
Grade 2 – Also called as Second Degree Piles. Piles protrudes during the passage of stool but recede back on its own. Bleeding, itching, and discomfort are common symptoms at this stage.
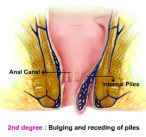
Fig 5: 2nd Degree Piles
Grade 3 – Also known as Third Degree Piles. The protrusion does not recede back on its own as the piles prolapse upon pressure. It has to be push back in by hand. They might stay outside the anus and can cause significant discomfort, pain, bleeding, and itching.
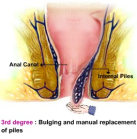
Fig 6: 3rd Degree Piles
Grade 4 – Also known as Fourth Degree Piles. Piles may protrude any time of the day and remains permanently protruded. They need treatment or surgery (called a haemorrhoidectomy). They may lead to considerable pain, bleeding, itching, and difficulty in hygiene maintenance.
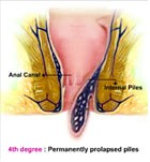
Fig 7: 4th Degree Piles
What causes Haemorrhoids or piles?
An exact cause is unknown; however, the upright posture of humans alone forces a great deal of pressure on the rectal veins. Piles, or Haemorrhoids, develop when there is increased pressure on the veins in the rectum and anus. This pressure causes the veins to swell and become inflamed. Whatever the cause, the tissues supporting the vessels stretch. As a result, the vessels dilate; their walls become thin and bleed. If the stretching and pressure continue, the weakened vessels protrude.
There are several other contributing factors causing piles, and understanding them can help manage and prevent the condition. These include:
- Age: As individuals get older, their risk of developing haemorrhoids increases. This is due to the weakening of the connective tissues in the rectal and anal area.
- Chronic Constipation and Diarrhoea: Both chronic constipation and frequent bouts of diarrhoea can irritate the rectal area leading to straining. The extra pressure on the rectal veins contribute to haemorrhoid formation.
- Straining during bowel movements: This is one of the most common causes, often associated with constipation.
- Faulty bowel function due to overuse of laxatives or enemas.
- Prolonged Toilet Sitting: Sitting on the toilet for an extended period, especially when straining during bowel movements, can increase the pressure on the rectal veins, potentially leading to haemorrhoids.
- Obesity: Excess body weight can put additional strain on the rectal and anal areas, making it more likely for haemorrhoids to develop.
- Lack of Fibre in the Diet: A diet low in fibre can lead to constipation, increasing the risk of haemorrhoids. Fibre helps soften the stool, making it easier to pass.
- Sedentary lifestyle: Lack of physical activity can result in poor circulation and contribute to the development of piles.
- Pregnancy: During pregnancy, the growing uterus puts increased pressure on the veins in the rectum, leading to piles. The growing uterus and hormonal changes can be contributing factors. Hormonal changes and constipation also contribute to the development of Haemorrhoids in pregnant women.
- Heredity or Genetic predisposition: A family history of piles can increase the likelihood of developing the condition.
- Lifting Heavy Weights: Straining while lifting heavy objects can lead to increased abdominal pressure, which can, in turn, strain the veins in the rectal area.
- Prolonged Sitting or Standing: Jobs or lifestyles that involve long hours of sitting or standing without breaks can also contribute to the development of haemorrhoids.
Yet other factors include:
- Colon malignancy
- Hepatic disease
- Anticoagulant or antiplatelet therapy
- Elevated anal resting pressure
- Spinal cord injury
- Loss of rectal muscle tone
- Rectal surgery
- Episiotomy
- Anal intercourse
- Inflammatory bowel disease, including ulcerative colitis and Crohn disease
Signs and Symptoms of Piles
Haemorrhoids can lead to various symptoms that depend on their classification (internal or external) and intensity. Identifying these symptoms promptly can assist in obtaining timely care.
Here are some common symptoms of piles:
- Itchy Anus: Piles can cause ongoing itching in the anal region, often resulting from irritation and inflammation.
- Bleeding: A key indication is the presence of blood in the toilet bowl following a bowel movement, on toilet paper, or even mixed within the stool. This bleeding can vary from slight spotting to more substantial amounts.
- Pain: Haemorrhoids can be painful, particularly when sitting or during bowel movements. This discomfort can range in severity.
- Hard or Tender Lumps: Individuals may feel firm or sensitive lumps around or on the anus. These lumps are typically swollen blood vessels linked to haemorrhoids.
- Swelling or a lump near the anus: Commonly related to external piles, these lumps may be painful or tender.
- Mucus discharge: This may happen after a bowel movement, causing additional irritation.
If you notice any of these haemorrhoid symptoms, it is important to consult a healthcare professional. Early identification and treatment can ease discomfort and help prevent complications.
Diagnosis of Piles (Haemorrhoids)
If you experience the symptoms mentioned above, you might be suffering from piles; however, it is essential to be careful as not all rectal bleeding is solely due to piles. Bleeding could indicate a more serious condition such as cancer. Therefore, consulting a doctor, ideally a surgeon, for diagnosis is crucial. Haemorrhoids can typically be identified by evaluating a patient’s medical history and performing physical examinations. In some cases, they may also be diagnosed through a digital rectal examination, which involves a gloved, lubricated finger to feel for them. External piles can be seen, but for internal haemorrhoids, physicians might examine the intestinal tract using various tests.
Typical Tests
Certain diagnostic examinations that assist physicians in determining whether a patient has haemorrhoids include anoscopy, sigmoidoscopy, and colonoscopy. These methods utilise a scope to visualise the intestines, colon, rectum, and anus. Anoscopy and sigmoidoscopy generally do not need anaesthesia or sedatives, while a colonoscopy might necessitate some sedatives or anaesthesia.
- Physical Examination – External Haemorrhoids or lumps around the anus can often be visually assessed by the doctor. This initial examination helps identify external piles and any associated swelling or thrombosis.
- Digital Rectal Exam – This exam involves the doctor inserting a gloved finger into the rectum to feel for any abnormalities or internal Haemorrhoids. It helps detect swollen veins and any signs of inflammation.
- Anoscopy or Proctoscopy – These are procedures that use a small tube with a light (anoscope or proctoscope) to view the anal canal and lower rectum. They provide a clear view of internal piles and help assess their size, location, and degree of prolapse.
- Colonoscopy – A colonoscopy may be recommended for individuals over the age of 50 or those with a family history of colorectal cancer. It allows for a more comprehensive examination of the colon and rectum to rule out other conditions and ensure the piles aren’t a sign of more serious problems.
By using these methods, a colorectal surgeon can accurately diagnose the presence of piles and determine the best course of treatment.
Complications of Haemorrhoids
- Profuse bleeding
- Thrombosis
- Strangulation
- Ulceration of haemorrhoids
- Pylephlebitis
- Suppuration
- Gangrene
Treatment of Haemorrhoids (Piles)
There are various methods of managing haemorrhoids. The main aim is to relieve the symptoms, correct the precipitating factor and to reduce the risk of relapse. The treatment for piles (Haemorrhoids) can vary depending on the severity and type (internal or external). Haemorrhoid’s treatment includes a combination of at-home care and, if necessary, medical procedures & surgeries. Procedures and surgeries are for cases where there is a disruption in a person’s everyday activities. General lifestyle modification and dietary changes goes a long way in not only reducing the symptoms but preventing relapse too.
Home Remedies for Piles
For mild cases, lifestyle changes and home treatments can help alleviate symptoms:
- High-Fiber Diet: Incorporating foods like fruits, vegetables, and whole grains helps soften stool and reduces straining during bowel movements, which is a key contributor to piles.
- Hydration: Drinking plenty of water ensures stool remains soft, preventing constipation and reducing the risk of Haemorrhoids.
- Warm Sitz Baths: Soaking the anal area in warm water for 10-15 minutes can help relieve discomfort and reduce swelling.
- Over-the-Counter Creams: Products containing hydrocortisone or witch hazel can soothe itching, swelling, and irritation around the anus.
With these measures, the pain and swelling of most symptomatic Haemorrhoids will decrease in two to seven days, and the firm lump should recede within four to six weeks. In cases of severe or persistent pain from a thrombosed-piles, your colorectal surgeon may elect to remove it containing the clot with a small incision. Performed under local anaesthesia, this procedure generally provides relief.
Common Procedures for Piles Treatment
- Medications: May include laxatives to relieve constipation, pain relievers to reduce discomfort, or topical treatments to reduce inflammation and soothe irritation.
- Rubber Band Ligation – The surgeon binds the base of the haemorrhoids with rubber bands to cut off the blood supply. The haemorrhoids fall off in a week, making it an effective treatment plan. The chance of recurrence is less than 5%.
- Infrared Coagulation – It uses infrared light to heat a blood vessel and cut off the blood supply.
- Electrocoagulation – This treatment method uses an electric current that causes the proteins in the affected tissue to coagulate/clot, thus killing the tissue.
- Sclerotherapy – One can consider haemorrhoids to be the varicose veins that affect the bottom. Similarly, to varicose veins, a solution is injected into the affected area to shrivel the veins, which eventually become scar tissue.
Surgical Interventions for Piles
For severe or prolapsed Haemorrhoids that don’t respond to other treatments, surgery may be required:
- Haemorrhoidectomy: This is a surgical procedure where the Haemorrhoids are removed, typically recommended for large or persistent piles.
- Stapled Haemorrhoidopexy: A surgical option used for prolapsed piles, where the Haemorrhoids are stapled back into place and excess tissue is removed.
- Laser Treatment for Piles: A minimally invasive option that uses a laser to shrink the Haemorrhoids, offering a faster recovery compared to traditional surgery.
These treatment options provide various solutions depending on the severity of the Haemorrhoids. For personalized recommendations, it’s essential to consult with a healthcare professional to determine the most appropriate treatment for your condition.
Prevention of Piles
To reduce the risk of developing piles (Haemorrhoids), it’s important to adopt a few healthy lifestyle habits. Here are some effective ways to prevent piles:
- Maintain a High-Fibre Diet – A high-fibre diet, rich in fruits, vegetables, and whole grains, helps soften stools, making bowel movements easier and reducing the risk of constipation and straining.
- Stay Hydrated – Drinking plenty of water keeps the stool soft and reduces the chances of constipation, which can lead to piles.
- Avoid Prolonged Sitting or Standing – Sitting or standing for extended periods puts pressure on the veins in the rectal area. Take breaks to walk around and avoid prolonged periods of immobility.
- Exercise Regularly – Regular physical activity improves blood circulation and digestion, helping to prevent constipation and reduce the risk of Haemorrhoids.
- Avoid Straining During Bowel Movements – Straining while passing stool can lead to increased pressure on the rectal veins. To prevent straining, don’t delay bowel movements, and make sure you pass stool when the urge arises.
- Use the Correct Posture While Using the Toilet – Avoid sitting on the toilet for long periods. If necessary, use a footstool to elevate your feet slightly, which can help reduce strain during bowel movements.
- Maintain a Healthy Weight – Being overweight or obese increases the risk of developing piles due to the increased pressure on the abdominal area. Maintaining a healthy weight can help prevent Haemorrhoids.
- Avoid Lifting Heavy Weights – Lifting heavy weights or engaging in strenuous activities that put pressure on the abdominal area can increase the risk of Haemorrhoids. If necessary, use proper lifting techniques to minimize strain.
By incorporating these habits into your lifestyle, you can significantly reduce the risk of developing piles and manage symptoms effectively.

